
💡 What You Need to Know Right Away
A shoulder MRI is a diagnostic imaging test that uses magnetic fields and radio waves to create detailed pictures of bones, tendons, muscles, and blood vessels in your shoulder, helping doctors detect rotator cuff tears, labral injuries, tendonitis, and inflammation without using any radiation.
Also known as: shoulder MRI scan, MR imaging of the shoulder, magnetic resonance imaging of shoulder joint
- Research shows shoulder MRI correctly identifies full-thickness rotator cuff tears in about 8 out of 10 cases[Evidence: A][1]
- The scan takes 30-45 minutes (standard protocol) or as little as 7 minutes with newer deep learning technology[Evidence: B][3]
- MRI uses no radiation, making it safe for repeated imaging when needed
- Clinical guidelines recommend MRI as the appropriate test when rotator cuff tear is suspected[Evidence: D][10]
If your doctor has recommended a shoulder MRI, you probably have questions. What will it feel like? How long does it take? Will it hurt? It is common to feel anxious about medical imaging tests, especially if you have never had an MRI before or worry about enclosed spaces.
The good news is that shoulder MRI is a painless, radiation-free test that gives doctors detailed information about soft tissues like tendons, ligaments, and cartilage. Unlike X-rays, which mainly show bones, MRI reveals the structures most often involved in shoulder pain and injury.
In this guide, you will learn exactly what to expect before, during, and after your shoulder MRI. We cover preparation steps, the scanning procedure itself, how to manage claustrophobia, understanding your results, and what costs to anticipate. Our goal is to help you feel calm and informed.
❓ Quick Answers
Is shoulder MRI safe?
Shoulder MRI is very safe because it uses magnetic fields and radio waves instead of radiation. There is no exposure to X-rays or ionizing radiation. The main considerations are metal implants (some are not MRI-compatible) and contrast dye allergies if your scan requires contrast injection.
How long does a shoulder MRI take?
A standard shoulder MRI takes 30-45 minutes of active scanning time. Including check-in, changing, and positioning, plan for about 60-90 minutes total at the imaging center. Newer facilities using deep learning acceleration can complete scans in as little as 7 minutes[Evidence: B][3].
Is shoulder MRI painful?
The MRI scan itself is painless. You will not feel the magnetic field or radio waves. However, lying still for 30-45 minutes with your arm in a specific position can be uncomfortable, especially if your shoulder is already injured. If contrast dye is used, you may feel a brief pinch from the IV insertion.
What can a shoulder MRI detect?
Shoulder MRI detects rotator cuff tears (full and partial thickness), labral tears including SLAP lesions, tendonitis, bursitis, frozen shoulder (adhesive capsulitis)[Evidence: B][5], biceps tendon problems[Evidence: C][7], arthritis, fractures, and tumors.
Do I need to fast for shoulder MRI?
No fasting is required for a standard shoulder MRI without contrast. If your scan involves contrast dye injection, your imaging center may request you avoid eating for 2-4 hours beforehand to reduce nausea risk. Always follow your specific facility's instructions.
How much does a shoulder MRI cost?
Shoulder MRI costs range from $500 to $4,000 depending on your location, facility type, and insurance coverage. Hospital-based MRI typically costs more than outpatient imaging centers. With insurance, expect to pay $100-$900 depending on your deductible and copay.
When should I get an MRI for shoulder pain?
Clinical guidelines recommend MRI when you have acute shoulder pain with dislocation or instability, or when rotator cuff tear is suspected[Evidence: D][10]. Your doctor may also order MRI after 6 weeks of conservative treatment (physical therapy, rest) if pain persists.
Shoulder MRI
A comprehensive visual guide to Magnetic Resonance Imaging of the shoulder complex. Understanding the procedure, indications, and what the technology reveals about your joint health.
🔬 How Does Shoulder MRI Work?
MRI technology works by using powerful magnets and radio waves to create detailed images of structures inside your body. Think of it like this: your body contains billions of hydrogen atoms, and the MRI scanner acts like a conductor leading an orchestra, temporarily aligning these atoms using its magnetic field. When the field pulses, the atoms release tiny signals that a computer translates into highly detailed images.
Unlike X-rays and CT scans, which excel at showing bones, MRI provides superior images of soft tissues. This makes it ideal for evaluating the tendons, ligaments, cartilage, and muscles that make up your shoulder's rotator cuff and supporting structures.
What Makes Shoulder MRI Different?
During a shoulder MRI, the scanner takes images from multiple angles. Radiologists use different image "sequences" called T1-weighted and T2-weighted images. Think of these like different camera filters: T1 images highlight anatomical structure (the "what"), while T2 images reveal fluid and inflammation (the "where something is wrong"). Injuries often show as bright white areas on T2 images because damaged tissue accumulates fluid.
Research shows that standard MRI correctly identifies full-thickness rotator cuff tears with sensitivity of 84% and specificity of 86%[Evidence: A][1]. For labral tears (cartilage rim damage), standard MRI sensitivity ranges from 74-83%[Evidence: A][2].
MRI With Contrast (MR Arthrography)
Sometimes doctors order MRI with contrast dye injected directly into the shoulder joint. This technique, called MR arthrography, improves detection of labral tears to over 94-98% sensitivity[Evidence: A][2]. The contrast fluid distends the joint, making small tears easier to see. Studies show MR arthrography sensitivity of 98% compared to 76% for standard MRI[Evidence: B][6].
🧪 What to Expect: The Real User Experience
During the Procedure
You will lie on a narrow table with your shoulder positioned flat and your arm parallel to your body. Foam cushions are placed around your shoulder for stability, and a lightweight plastic frame called a shoulder coil (weighing about 2 pounds) sits over your shoulder to capture the signals.
The table slides into a tunnel that is typically 60 centimeters (about 24 inches) in diameter for standard scanners, or 70 centimeters (28 inches) for wide-bore MRI machines. Your head, shoulders, and upper torso enter the tunnel, but your lower body remains outside. The room is kept cool at 65-68°F to prevent scanner overheating, so you may feel cold in the hospital gown.
The machine makes loud banging and knocking sounds during scanning. Noise levels range from 95-130 decibels, comparable to a jackhammer. This sound is intermittent, not continuous. You will receive ear protection (earplugs or headphones), and many facilities offer music to help pass the time.
What You'll Feel After
Most people experience mild shoulder stiffness from lying still, which resolves within 1-2 hours. If contrast dye was used, you may notice a metallic taste lasting 15-30 minutes. Ear ringing can occur if ear protection was inadequate, but this is typically temporary. You can resume normal activities immediately unless you received sedation for claustrophobia.
How to Make It Easier
- For the noise: Request both earplugs AND headphones for dual protection (reduces noise by 20-30 dB). Ask if they offer music playlists.
- If claustrophobic: Keep your eyes closed before entering the tunnel. Bring an eye mask or ask for a washcloth to cover your eyes.
- To stay calm: Practice 4-7-8 breathing beforehand (inhale 4 counts, hold 7, exhale 8). You can hold a squeeze ball to alert the technologist if needed.
- For positioning comfort: Ask the technologist to elevate your elbow with extra cushions to reduce strain on an injured rotator cuff.
- Sedation option: If you have severe claustrophobia, discuss oral or IV sedation with your doctor 1-2 weeks before your appointment. You will need a driver afterward.
📋 Preparation and Procedure
Before Your Appointment
Preparing for a shoulder MRI is straightforward. Unlike some medical tests, no fasting is required for standard MRI. If your scan includes contrast dye, your facility may ask you to avoid eating for 2-4 hours before.
| Category | What to Do | Why It Matters |
|---|---|---|
| What to Wear | Loose clothing without metal zippers, snaps, or underwire. You may change into a gown. | Metal interferes with imaging and can heat up in the magnetic field |
| What to Bring | Photo ID, insurance card, referral order, implant information card if applicable | Required for registration and safety screening |
| What to Remove | Jewelry, watches, hearing aids, hairpins, credit cards, phones | Strong magnet can damage electronics and pull metal objects |
| What to Disclose | All implants, previous surgeries, metal fragments, tattoos, pregnancy status | Some implants are not MRI-safe; safety screening prevents injury |
Scan Duration by Type
| MRI Type | Scan Time | Total Visit Time | Evidence |
|---|---|---|---|
| Standard Shoulder MRI | 30-45 minutes | 60-90 minutes | [Evidence: A][1] |
| MRI with Contrast | 45-60 minutes | 90-120 minutes | [Evidence: B][6] |
| Deep Learning Accelerated MRI | 7-15 minutes | 30-45 minutes | [Evidence: B][3] |
Newer facilities using deep learning technology can reduce scan time by 50% while maintaining 98-100% sensitivity[Evidence: B][4]. Ask your imaging center if accelerated protocols are available.
⚠️ Safety and Considerations
Shoulder MRI is one of the safest imaging tests available. It uses no ionizing radiation, making it suitable for repeated imaging when needed. The scan itself is painless, though the narrow tunnel may feel confining and the machine makes loud knocking sounds. It is normal to feel anxious about medical tests, but most people tolerate MRI well with proper preparation.
Who Should Not Have MRI
Absolute contraindications include non-MRI-conditional cardiac pacemakers, implantable defibrillators, metallic intraocular foreign bodies, and certain ferromagnetic aneurysm clips. If you have any implanted device, provide documentation of its MRI compatibility status.
Contrast Dye Considerations
If your scan requires gadolinium contrast (IV or joint injection), inform staff if you have kidney disease, previous contrast reactions, or are breastfeeding. Common temporary effects include coolness or warmth sensation when dye enters the bloodstream (5-10 seconds) and metallic taste (15-30 minutes). Serious reactions are rare but require immediate attention.
🥗 Practical Recommendations
When to Get a Shoulder MRI
Clinical guidelines recommend shoulder MRI in specific situations[Evidence: D][10]:
- Acute shoulder pain with dislocation or instability: MRI is usually appropriate to assess labral and ligament damage
- Suspected rotator cuff tear: Especially if you have weakness lifting your arm or significant pain with overhead movements
- After 6 weeks of conservative treatment: If physical therapy, rest, and medication have not improved symptoms
- Before surgery: To plan the surgical approach and identify all areas of damage
For initial evaluation of shoulder pain without red flags, X-rays are typically ordered first[Evidence: D][10]. MRI is reserved for cases where soft tissue injury is suspected or X-rays do not explain symptoms.
Reducing Costs
- Use outpatient imaging centers: Typically 40-60% less expensive than hospital-based MRI
- Ask about cash-pay discounts: Many facilities offer 20-40% off for upfront payment
- Verify insurance authorization: Ensure your scan is pre-approved to avoid surprise bills
- Compare facility prices: Prices can vary 3-5x for the same scan in the same city
Understanding Your Results
A radiologist (imaging specialist) interprets your MRI and sends a report to your ordering doctor. Results are typically available within 1-2 business days. If findings are abnormal, your doctor will discuss next steps, which may include referral to an orthopedic surgeon, physical therapy, or additional imaging.
What to Look for When Choosing a Shoulder MRI Provider
The quality of your test results depends on the imaging facility and equipment used. Here is what to consider:
Quality Markers
- CLIA certification: Required for all diagnostic imaging labs Why it matters: Federal quality standards ensure accurate results
- ACR accreditation: American College of Radiology accreditation indicates rigorous quality standards Why it matters: ACR-accredited facilities meet strict equipment and personnel requirements
- Magnet strength: 3-Tesla (3T) MRI provides higher resolution than 1.5T for shoulder imaging[Evidence: A][2] Why it matters: Higher field strength improves detection of small tears
- Radiologist specialization: Fellowship-trained musculoskeletal radiologists provide specialized interpretation Why it matters: Subspecialty training improves diagnostic accuracy
- Wide-bore option: 70cm bore reduces claustrophobia compared to standard 60cm Why it matters: More comfortable for anxious patients
Questions to Ask Your Provider
- What is your magnet strength (1.5T or 3T)?
- Are your radiologists fellowship-trained in musculoskeletal imaging?
- Do you offer wide-bore MRI for claustrophobic patients?
- What is the typical turnaround time for results?
- What is the cost with my insurance? Without insurance?
- Do you offer music or other comfort amenities during the scan?
Red Flags to Avoid
- No ACR accreditation: Lack of professional accreditation indicates lower quality standards
- Unusually low prices: May indicate older equipment or less experienced radiologists
- No option to discuss results: Quality facilities ensure your doctor receives and reviews your report
- Pressure to add unnecessary tests: Your ordering doctor should determine what imaging you need
Shoulder MRI vs CT vs X-ray: Which Is Right for You?
MRI, CT, and X-ray each have specific strengths for evaluating shoulder problems. Your doctor chooses based on what they need to see. Here is how they compare:
| Feature | MRI | CT Scan | X-ray |
|---|---|---|---|
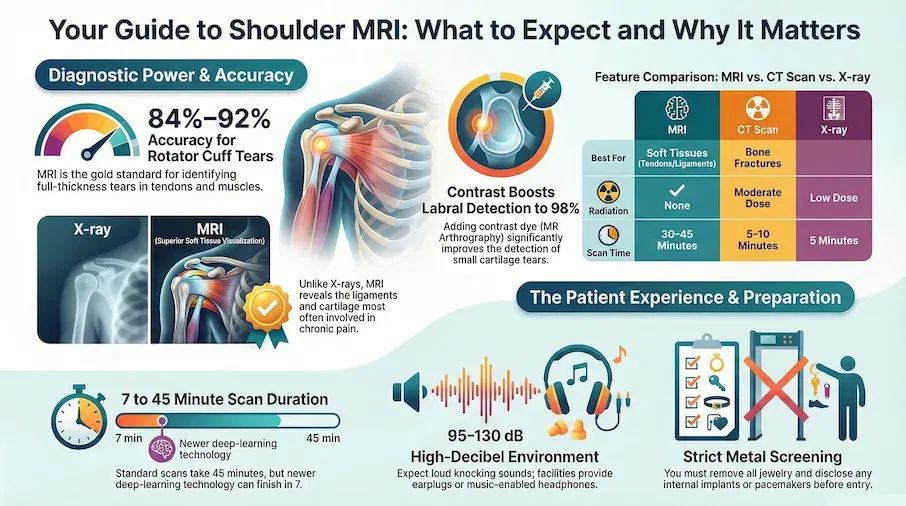
| Best for | Soft tissues (tendons, ligaments, cartilage, muscles) | Bones and fractures, complex fracture patterns | Initial screening, obvious fractures, arthritis |
| Radiation | None | Yes (moderate dose) | Yes (low dose) |
| Rotator cuff tear detection | 84-92% sensitivity[Evidence: A][1] | Limited (soft tissue detail) | Cannot detect directly |
| Labral tear detection | 74-98% sensitivity[Evidence: A][2] | Poor (requires arthrography) | Cannot detect |
| Scan time | 30-45 minutes | 5-10 minutes | 5 minutes |
| Cost (without insurance) | $500-$4,000 | $300-$1,500 | $100-$300 |
| Claustrophobia risk | Higher (enclosed tunnel) | Lower (open design) | None |
MRI With Contrast vs Without Contrast
Standard MRI (without contrast) is appropriate for most rotator cuff evaluations. MR arthrography (with contrast injected into the joint) provides superior detection of labral tears and partial-thickness rotator cuff tears.
| Feature | MRI Without Contrast | MRI With Contrast (MR Arthrography) |
|---|---|---|
| Procedure | No injection required | Contrast injected into joint under fluoroscopy |
| Rotator cuff detection | 76% sensitivity[Evidence: B][6] | 98% sensitivity[Evidence: B][6] |
| Labral tear detection | 74-83% sensitivity[Evidence: A][2] | 94-98% sensitivity[Evidence: A][2] |
| Best for | Full-thickness tears, general assessment | Labral tears, partial tears, instability workup |
| Additional cost | Baseline | +$100-$300 for contrast and injection |
What The Evidence Shows (And Doesn't Show)
What Research Suggests
- Shoulder MRI correctly identifies full-thickness rotator cuff tears in 84-92% of cases, with specificity of 86-98% (based on a network meta-analysis of 144 studies with 14,059 patients)[Evidence: A][1]
- MR arthrography (contrast injected into joint) achieves 94-98% sensitivity for labral tears, significantly outperforming standard MRI at 74-83%[Evidence: A][2]
- Deep learning accelerated MRI protocols can reduce scan time by 50% while maintaining 95-100% sensitivity[Evidence: B][4]
- MRI correctly identifies frozen shoulder (adhesive capsulitis) in 84% of cases with 94% specificity[Evidence: B][5]
What's NOT Yet Proven
- Partial-thickness rotator cuff tears have lower detection rates (65-78%) on standard MRI[Evidence: C][7]. MR arthrography may be needed for suspected partial tears with negative standard MRI
- SLAP lesion detection varies widely (60-93%) depending on imaging protocol, magnet strength, and radiologist experience
- Deep learning accelerated protocols, while promising, represent emerging technology with broader validation ongoing
- Long-term outcomes comparing patients who had MRI-guided treatment versus clinical diagnosis alone are limited
Where Caution Is Needed
- Biceps pulley lesions have lower detection rates (65-78% sensitivity) on standard MRI[Evidence: C][7]
- Posterior labral tears are particularly challenging, with only 57% sensitivity even with MR arthrography[Evidence: C][9]
- Image quality varies by facility, magnet strength, and protocol. A negative MRI does not definitively rule out injury
- Overreliance on MRI findings can lead to unnecessary surgery. Clinical correlation is essential
Should YOU Get This Test?
Best suited for: People with persistent shoulder pain unresponsive to 6 weeks of conservative treatment, suspected rotator cuff tears (weakness, pain with overhead movements), shoulder instability or dislocation, and pre-surgical planning.
May not be needed for: Mild shoulder pain of recent onset, clear traumatic fracture (X-ray sufficient), or when treatment plan will not change regardless of MRI findings.
Expected timeline: Schedule within 1-2 weeks. Scan takes 30-60 minutes. Results available in 1-2 business days.
When to consult a professional: If you have implanted devices, kidney disease (for contrast scans), severe claustrophobia requiring sedation, or pregnancy. Always discuss MRI necessity and findings with your healthcare provider.
Frequently Asked Questions
Can I have a shoulder MRI if I have metal implants?
It depends on the type of implant. Most modern orthopedic hardware (joint replacements, screws, plates) is MRI-compatible. However, older implants, pacemakers, implantable defibrillators, cochlear implants, and certain aneurysm clips may not be safe. Always bring documentation of your implant's MRI compatibility. The imaging center will screen you before the scan and may contact your surgeon if needed. When in doubt, ask your doctor to verify implant safety before scheduling.
How long until I get my shoulder MRI results?
Results are typically available within 1-2 business days. A radiologist interprets the images and sends a written report to your ordering doctor. Your doctor then reviews the findings and contacts you to discuss results and next steps. If you have an urgent concern, ask your doctor if they can expedite the reading. Some imaging centers offer online patient portals where you can view your report, though you should always discuss findings with your doctor for proper interpretation.
What if I feel claustrophobic during the MRI?
Claustrophobia affects about 15% of MRI patients. Several strategies help: keep your eyes closed before entering the tunnel, use an eye mask, practice deep breathing techniques beforehand, request music through headphones, and use the squeeze ball buzzer if you need a break. The technologist can communicate with you throughout the scan via intercom. For severe anxiety, ask your doctor about oral sedation (taken 30-60 minutes before) or IV sedation. Wide-bore MRI machines (70cm vs 60cm diameter) also reduce claustrophobia significantly.
Do I need a referral for a shoulder MRI?
In most cases, yes. Insurance companies typically require a physician's order for MRI to be covered. Your primary care doctor or orthopedic surgeon evaluates your symptoms, examines your shoulder, and determines if MRI is medically necessary. Some insurance plans also require prior authorization (pre-approval) before the scan. Without insurance, some imaging centers accept self-pay patients without a referral, though having a doctor to interpret results and guide treatment is strongly recommended.
Can shoulder MRI detect arthritis?
Yes, MRI can detect arthritis changes including cartilage loss, bone spurs, joint space narrowing, and inflammation of the joint lining (synovitis). However, X-rays are typically the first choice for arthritis evaluation because they are faster, cheaper, and effectively show bone changes. MRI is more useful when your doctor suspects soft tissue problems (rotator cuff, labrum) alongside arthritis, or when X-ray findings do not match your symptoms.
What is the difference between open MRI and closed MRI for shoulder?
Closed MRI uses a tunnel design (60-70cm diameter) and produces higher-resolution images. Open MRI has open sides, eliminating claustrophobia but using weaker magnets (typically 0.3-0.7T vs 1.5-3T). For shoulder imaging, closed MRI is preferred because detecting small rotator cuff tears and labral injuries requires the higher resolution of stronger magnets. Wide-bore closed MRI (70cm) offers a compromise: better image quality than open MRI with reduced claustrophobia compared to standard closed MRI.
How accurate is MRI for detecting SLAP tears?
SLAP tears (Superior Labral tear from Anterior to Posterior) are among the more challenging shoulder injuries to detect. Standard MRI correctly identifies SLAP tears in about 60-93% of cases when present, with higher accuracy for complete tears. MR arthrography improves detection to about 75-84% sensitivity. Using a special arm position called ABER (Abduction External Rotation) during the scan can also improve detection.
Can I drive after a shoulder MRI?
Yes, you can drive immediately after a standard shoulder MRI without sedation. The scan does not involve radiation, anesthesia, or medications that impair driving ability. However, if you received sedation for claustrophobia (oral or IV), you must have someone drive you home. Sedation effects can last several hours, making it unsafe to drive, operate machinery, or make important decisions. Plan ahead if you know sedation will be needed.
Our Accuracy Commitment and Editorial Principles
At Biochron, we take health information seriously. Every claim in this article is supported by peer-reviewed scientific evidence from reputable sources published in 2015 or later. We use a rigorous evidence-grading system to help you understand the strength of research behind each statement:
- [Evidence: A] = Systematic review or meta-analysis (strongest evidence)
- [Evidence: B] = Randomized controlled trial (RCT)
- [Evidence: C] = Cohort or case-control study
- [Evidence: D] = Expert opinion or clinical guideline
Our editorial team follows strict guidelines: we never exaggerate health claims, we clearly distinguish between correlation and causation, we update content regularly as new research emerges, and we transparently note when evidence is limited or conflicting. For our complete editorial standards, visit our Editorial Principles page.
This article is for informational purposes only and does not constitute medical advice. Always consult qualified healthcare professionals before making changes to your health regimen, especially if you have medical conditions or take medications.
References
- 1 . Detecting Rotator Cuff Tears: A Network Meta-analysis of 144 Diagnostic Studies, Orthopaedic Journal of Sports Medicine, 2020, Liu F et al., PubMed [Evidence: A]
- 2 . Diagnosis of glenoid labral tears using 3-tesla MRI vs. 3-tesla MRA: a systematic review and meta-analysis, Archives of Orthopaedic and Trauma Surgery, 2018, Ajuied A et al., PubMed [Evidence: A]
- 3 . Arthroscopy-validated Diagnostic Performance of 7-Minute Five-Sequence Deep Learning Super-Resolution 3-T Shoulder MRI, Radiology, 2025, Vosshenrich J et al., PubMed [Evidence: B]
- 4 . Deep Learning-Driven Abbreviated Shoulder MRI Protocols: Diagnostic Accuracy in Clinical Practice, Tomography, 2025, Foti G et al., PubMed [Evidence: B]
- 5 . Diagnostic accuracy of non-contrast MRI in frozen shoulder, Archives of Orthopaedic and Trauma Surgery, 2024, de Angelis Guerra Dotta T et al., PubMed [Evidence: B]
- 6 . Evaluation of Shoulder Injuries: A Comparative Study of Imaging by Magnetic Resonance Imaging (MRI) and Magnetic Resonance Arthrography (MRA), Journal of Pharmacy & Bioallied Sciences, 2024, Dwivedi A et al., PubMed [Evidence: B]
- 7 . Biceps Pulley Lesions: Diagnostic Accuracy of Nonarthrographic Shoulder MRI and the Value of Various Diagnostic Signs, Journal of Magnetic Resonance Imaging, 2024, Nada MG et al., PubMed [Evidence: C]
- 8 . Correlation Between Clinical Diagnosis, MRI, and Arthroscopy in Diagnosing Shoulder Pathology, Cureus, 2021, Thiagarajan A et al., PubMed [Evidence: C]
- 9 . Comparison of magnetic resonance arthrography with arthroscopy for imaging of shoulder injuries: retrospective study, Annals of the Royal College of Surgeons of England, 2017, Saqib R et al., PubMed [Evidence: C]
- 10 . ACR Appropriateness Criteria® Acute Shoulder Pain: 2024 Update, Journal of the American College of Radiology, 2025, Expert Panel on Musculoskeletal Imaging, PubMed [Evidence: D]
Medical Disclaimer
This content is for informational and educational purposes only. It is not intended to provide medical advice or to take the place of such advice or treatment from a personal physician. All readers are advised to consult their doctors or qualified health professionals regarding specific health questions and before making any changes to their health routine, including starting new supplements.
Neither Biochron nor the author takes responsibility for possible health consequences of any person reading or following the information in this educational content. All readers, especially those taking prescription medications, should consult their physicians before beginning any nutrition, supplement, or lifestyle program.
If you have a medical emergency, call your doctor or emergency services immediately.






