
💡 What You Need to Know Right Away
A PET-MRI scan is an imaging test that combines positron emission tomography (PET) and magnetic resonance imaging (MRI) to detect cancer, brain tumors, epilepsy, and other conditions with superior soft-tissue detail and significantly less radiation than traditional PET-CT scans.
Also known as: PET/MRI, PET-MR, Hybrid PET-MRI, Simultaneous PET-MRI, Integrated PET-MRI
- Research shows PET-MRI correctly identifies cancer spread to lymph nodes in about 93% of cases, compared to 75% with PET-CT[Evidence: A][3]
- PET-MRI reduces radiation exposure by 83-90% compared to PET-CT, making it especially valuable for children and patients needing multiple scans[Evidence: D][23]
- In people with brain tumors after treatment, specialized PET-MRI scans help doctors distinguish true tumor progression from treatment-related changes[Evidence: B][21]
- Total appointment time is 2-3 hours, with actual scanning taking 30-45 minutes depending on the body area being examined
If your doctor has recommended a PET-MRI scan, you may be wondering what to expect and why this specific test was chosen. It is normal to feel anxious about medical imaging procedures, especially one that combines two advanced technologies.
A PET-MRI scan offers a unique advantage: it captures both how your cells are functioning (from PET) and detailed pictures of your organs (from MRI) in a single appointment. This gives your healthcare team more complete information while exposing you to significantly less radiation than older scanning methods.
In this guide, you will learn how PET-MRI works, what happens during the procedure, how to prepare, and what your results may show. Understanding the process ahead of time can help you feel more confident and calm on scan day.
❓ Quick Answers
What is a PET-MRI scan?
A PET-MRI scan is an imaging test that combines two technologies in one appointment. The PET component shows how your cells are working by tracking a safe radioactive sugar solution, while the MRI component creates detailed pictures of your organs using magnetic fields. Together, they help doctors detect and stage cancers, evaluate brain conditions, and plan treatments with exceptional accuracy.
Is PET-MRI scan safe?
PET-MRI is considered safe for most people. The radiation exposure from the PET component is low, approximately equivalent to 3 cross-country flights. Unlike PET-CT, PET-MRI uses no additional radiation from the MRI portion. In children with lymphoma, PET-MRI reduces radiation exposure by 83-90% compared to PET-CT[Evidence: D][23]. Certain people with metal implants or pacemakers cannot safely undergo MRI. Discuss any implants with your doctor beforehand.
How long does PET-MRI scan take?
Total appointment time is typically 2-3 hours. This includes check-in and safety screening (15-20 minutes), radiotracer injection and waiting period (60-90 minutes), and the actual scan (30-45 minutes depending on body area). You must remain still during the scan to ensure clear images.
What does PET-MRI detect?
PET-MRI detects a wide range of conditions. In people with gynecologic cancers, it helps find cancer that has spread to lymph nodes[Evidence: B][1]. It accurately stages endometrial cancer[Evidence: B][14] and helps localize seizure focus in people with difficult-to-control epilepsy[Evidence: B][25].
Can PET-MRI tell if brain tumor is growing back?
Yes. Studies suggest Fluciclovine scans combined with MRI help doctors distinguish true tumor progression from treatment effects better than standard imaging[Evidence: B][21]. Dynamic analysis of how sugar is processed over time helps doctors tell the difference between tumor growing back versus treatment-related changes[Evidence: B][20].
Do I need to combine PET with MRI or can I do them separately?
Studies suggest that using scans together is more accurate than using either scan by itself[Evidence: B][9]. The simultaneous acquisition provides perfectly aligned images and reduces total appointment time. However, PET-MRI availability is limited, so your doctor may recommend separate scans if a hybrid scanner is not accessible in your area.
PET-MRI vs PET-CT: Which is better?
Research shows PET-MRI correctly identified cancer spread to lymph nodes in about 93% of cases, compared to about 75% with PET-CT[Evidence: A][3]. PET-MRI provides superior soft-tissue detail for brain, liver, and pelvic imaging. PET-CT remains better for lung imaging and is more widely available. Your doctor will recommend the best option for your specific condition.
PET-MRI Scan Technology
A breakthrough in diagnostic imaging that combines the metabolic insights of PET with the structural precision of MRI. Explore how this dual-modality approach is transforming modern medicine.
🔬 How Does PET-MRI Work?
Think of a PET-MRI scan as having two photographers working together. The first photographer (PET) uses a special light that only glows where cells are most active, like cancer cells that burn more energy. The second photographer (MRI) creates a detailed map of all your organs and tissues. When you combine both photos, you get a complete picture showing exactly where problems are located within your body's structure.
The PET component works by tracking a radiotracer, typically FDG (fluorodeoxyglucose), a safe radioactive sugar solution injected into your bloodstream. Cancer cells and highly active tissues absorb more sugar than normal cells, so they "light up" on the PET scan. The MRI component uses powerful magnetic fields and radio waves to create detailed images of soft tissues without any radiation.
Unlike sequential scanning where you move between two machines, simultaneous PET-MRI captures both types of images at the same time. Clinical guidelines describe the advantage of taking both scan types simultaneously for people with mouth, jaw, and facial cancers[Evidence: D][29]. This perfect alignment helps doctors pinpoint abnormalities with precision.
Why Doctors Choose PET-MRI for Specific Conditions
Cancer Staging: In people with colorectal cancer, PET-MRI correctly identified lymph node spread in about 9 out of 10 cases[Evidence: A][3]. In people with liver tumors, digital PET-MRI provided additional helpful information beyond what standard PET-CT showed[Evidence: B][4]. In people with head and neck cancers, combining scan images from both methods was better than using either scan alone[Evidence: B][8].
Prostate Cancer: Studies suggest combining PSMA scans with MRI provides more accurate information about how far prostate cancer has spread locally[Evidence: B][2]. Women with HER2-positive breast cancer receiving chemotherapy saw early changes on these scans that helped predict treatment response[Evidence: B][13].
Brain Conditions: In people with difficult-to-control epilepsy, dual-tracer scans helped surgeons identify and outline the seizure focus more accurately before surgery[Evidence: B][25]. In people with memory problems, combining multiple MRI techniques with metabolism scans improved dementia diagnosis[Evidence: B][24]. In children with juvenile Huntington disease, simultaneous hybrid scans revealed specific brain patterns that may serve as disease markers[Evidence: C][27].
Surgical Planning: In people with overactive parathyroid glands, this scan helped surgeons plan better approaches for removing the problem gland[Evidence: B][6]. Whole-body scans helped doctors find cancer spread in soft tissue sarcoma[Evidence: C][18].
Early research suggests new targeted tracers show promise for specific cancers. For example, [68Ga]Ga-XH-06 showed promise for diagnosing liver cancer in an initial study of 8 patients[Evidence: C][17]. In people being evaluated for memory problems, blood flow measured by MRI matched well with sugar metabolism measured simultaneously by PET[Evidence: B][28].
🧪 What to Expect: The Real User Experience
During the Procedure
During the PET-MRI, you will lie on a narrow table that slides into a tunnel about 23-26 inches wide. This is narrower than a standard MRI (27-28 inches), which can trigger claustrophobic sensations in approximately 30% of patients. The room is kept cool at 65-68°F, and you may feel cold in your hospital gown. Blankets are offered but may interfere with positioning.
The MRI component produces loud knocking, banging, and thumping sounds ranging from 100-130 decibels, comparable to a power saw or jackhammer. These sounds occur in rhythmic patterns that change every 2-5 minutes as different imaging sequences run. Earplugs or headphones with music are provided, reducing noise by approximately 25 dB. The PET component is silent.
Foam supports will be placed around your head, arms, and body to maintain stillness during the 30-45 minute scan. The positioning feels snug but not painful. You must remain completely still to ensure clear images. If you have existing back or neck pain, lying still on the hard table may cause discomfort after 20-25 minutes.
What You Will Feel After
After the scan, you might notice mild temporary hearing sensitivity or ringing (tinnitus) that typically resolves within 1-2 hours. Stiffness or soreness in your back, shoulders, or neck from lying still is common. If contrast was used, metallic taste may persist 15-30 minutes. Expect increased urination in 2-4 hours as your body flushes the radiotracer through your kidneys. Drink 8-10 glasses of water within 24 hours to accelerate clearance.
How to Make It Easier
- For claustrophobia: Close your eyes before entering the tunnel to reduce visual anxiety triggers. Some facilities offer mirror systems so you can see outside.
- For the noise: Ask for headphones with your preferred music playlist. Many facilities allow this.
- To stay calm: Practice 4-7-8 breathing technique beforehand (inhale 4 counts, hold 7, exhale 8). You will have a communication button to signal the technologist if needed.
- For comfort: Request a foam wedge under your knees to reduce lower back strain. Use the bathroom immediately before the scan.
- If severely anxious: Discuss sedation options with your doctor beforehand. Mild sedatives can be prescribed for patients with severe claustrophobia.
- For the best images: Stay warm the day before your scan. Wear warm clothing to your appointment. Warmth keeps fat cells inactive, improving image clarity.
📊 Procedure Timeline and Preparation
Understanding the complete procedure timeline helps you plan your day and reduces anxiety about what comes next.
| Phase | Duration | What Happens | What You'll Experience |
|---|---|---|---|
| Check-in and Safety Screening | 15-20 minutes | Complete metal safety questionnaire, change into hospital gown, confirm no contraindications | Questions about implants, review of medical history |
| IV Placement and Radiotracer Injection | 10 minutes | Nurse places IV in arm or hand, injects FDG radiotracer | Brief pinch from needle; some feel warm, flushed sensation spreading from injection site |
| Waiting Period (Uptake Phase) | 60-90 minutes | Radiotracer distributes throughout your body and is absorbed by active cells | Must remain quiet and warm; no exercise; relaxation only |
| Positioning on Scan Table | 10-15 minutes | Technologist positions you with foam supports, provides earplugs/headphones | Lying flat, foam supports placed, communication button given |
| Active Scanning | 30-45 minutes | Table moves into scanner; PET and MRI images captured simultaneously | Loud knocking sounds, must stay completely still, cool temperature |
| Post-Scan Instructions | 5 minutes | Technologist removes IV, provides aftercare instructions | Safe to drive; drink extra fluids; no dietary restrictions |
Preparation Requirements
| Timeframe | Do This | Avoid This |
|---|---|---|
| 24 hours before | Eat high-protein, low-carbohydrate meals; stay warm; confirm appointment | Strenuous exercise; caffeine; high-sugar foods |
| 6 hours before | Stop eating solid foods; water is encouraged | Food, sugary drinks, chewing gum |
| Day of scan | Wear warm, comfortable clothing without metal; arrive 30 minutes early; bring list of medications | Metal jewelry, underwire bras, belts with metal buckles |
| At the facility | Disclose all implants and medical devices; use restroom before scan | Using your phone during uptake phase (stay still and quiet) |
Results Timeline: Results are typically available within 1-3 business days. Your referring physician will discuss findings and next steps with you.
⚠️ Safety, Side Effects, and Warnings
The PET-MRI scan itself is painless. You may feel a brief pinch when the IV needle enters your vein. The radiotracer injection may cause a warm, flushed feeling that spreads from the injection site and fades within 2-3 minutes. Most people tolerate the procedure well.
Radiation Exposure
The radiation from PET-MRI comes only from the PET component (the radiotracer). The MRI uses magnetic fields, not radiation. Total effective dose is approximately 3.6 mSv, equivalent to about 3 cross-country flights or one year of natural background radiation.
Clinical guidelines recommend hybrid imaging as part of precision medicine approaches for children with brain tumors[Evidence: D][22]. In children with lymphoma, this scan reduces radiation exposure by about 83-90% compared to the standard PET-CT scan[Evidence: D][23].
Common Side Effects
- Brief warmth or flushing during radiotracer injection (resolves in 2-3 minutes)
- Temporary hearing sensitivity after scan (resolves in 1-2 hours)
- Back or neck stiffness from lying still (temporary)
- Metallic taste if contrast used (resolves in 15-30 minutes)
- Small bruise at IV site (resolves in 24-48 hours)
Rare Side Effects
- Mild headache (5-10% of patients)
- Nausea (2-5% of patients)
- Dizziness (2-3% of patients)
- Allergic reaction to contrast dye (rare, delayed reactions can occur 1-6 hours post-scan)
Special Considerations
Pregnancy and Breastfeeding: PET-MRI is generally avoided during pregnancy, especially the first trimester. If you are breastfeeding, discuss with your doctor. You may need to pump and discard breast milk for 24 hours after the scan.
Diabetes: Blood sugar should be below 200 mg/dL for optimal image quality. Follow your doctor's instructions about insulin and diabetes medications.
🥗 Practical Preparation Guide
How to Use This Information in Your Planning
Day Before Your Scan: Eat high-protein, low-carbohydrate meals (eggs, fish, chicken, cheese). Avoid bread, pasta, rice, and sweets. Stay warm throughout the day. Keeping your body warm helps fat cells remain inactive, which improves image quality.
Morning of Your Scan: Stop eating 6 hours before your appointment. Continue drinking water. Take prescribed medications with small sips of water unless instructed otherwise. Wear warm, comfortable clothing without metal.
What to Bring: Insurance card, photo ID, list of current medications, list of previous imaging studies, comfortable reading material for the waiting period (no phones during uptake phase).
Common Mistakes to Avoid
- Exercising before the scan: Exercise increases muscle glucose uptake, which can affect image accuracy. Avoid strenuous activity for 24 hours before.
- Consuming caffeine: Caffeine affects blood sugar and metabolism. Avoid coffee, tea, and energy drinks for 24 hours before.
- Staying cold: Cold temperatures activate brown fat, which shows up on scans and can obscure results. Stay warm the day before and day of your scan.
- Arriving late: The uptake phase requires precise timing. Arriving late may require rescheduling.
- Forgetting to disclose implants: Metal implants can pose safety risks during MRI. Complete the safety questionnaire thoroughly.
After Your Scan
- Drink 8-10 glasses of water within 24 hours to flush the radiotracer
- You may resume normal eating immediately
- Driving is safe unless you received sedation
- Avoid close contact with pregnant women and infants for a few hours (precautionary)
- Results typically available in 1-3 business days
What to Look for When Choosing a PET-MRI Provider
The quality of your test results depends on the facility and equipment. PET-MRI availability is limited (approximately 30 systems in the US compared to over 1,600 PET-CT systems). Here is what to consider:
Facility Quality Markers
- ACR Accreditation: American College of Radiology accreditation for both PET and MRI Why it matters: Confirms quality standards, equipment calibration, and technologist training
- Academic Medical Center Affiliation: Major centers like Stanford, Memorial Sloan Kettering, Mayo Clinic, University of Maryland Why it matters: Higher procedure volume, experienced radiologists, latest equipment and protocols
- Hybrid Scanner Type: Simultaneous acquisition (not sequential) Why it matters: Simultaneous acquisition provides perfectly aligned images and shorter scan times
- Specialized Radiologists: Nuclear medicine physicians and neuroradiologists on staff Why it matters: Expert interpretation improves diagnostic accuracy
Questions to Ask Your Provider
- Is your facility ACR-accredited for both PET and MRI?
- Do you have a simultaneous PET-MRI scanner or sequential scanning?
- How many PET-MRI scans does your facility perform monthly?
- Who will interpret my results (nuclear medicine specialist, radiologist)?
- What is the turnaround time for results?
- Does my insurance cover PET-MRI at your facility?
- Do you offer sedation options for claustrophobia?
Red Flags to Avoid
- No accreditation information available: Legitimate facilities display accreditation status
- Unusually short appointment times: Quality PET-MRI requires 2-3 hours total
- No nuclear medicine physician review: Results should be interpreted by qualified specialists
- Pressure to schedule immediately without reviewing medical history: Proper screening is essential for safety
How PET-MRI Compares to PET-CT: What to Know
PET-MRI and PET-CT are both hybrid imaging technologies that combine metabolic information (from PET) with anatomical imaging (from MRI or CT). They use similar radiotracer technology but differ in how they create structural images and their clinical strengths.
| Feature | PET-MRI | PET-CT |
|---|---|---|
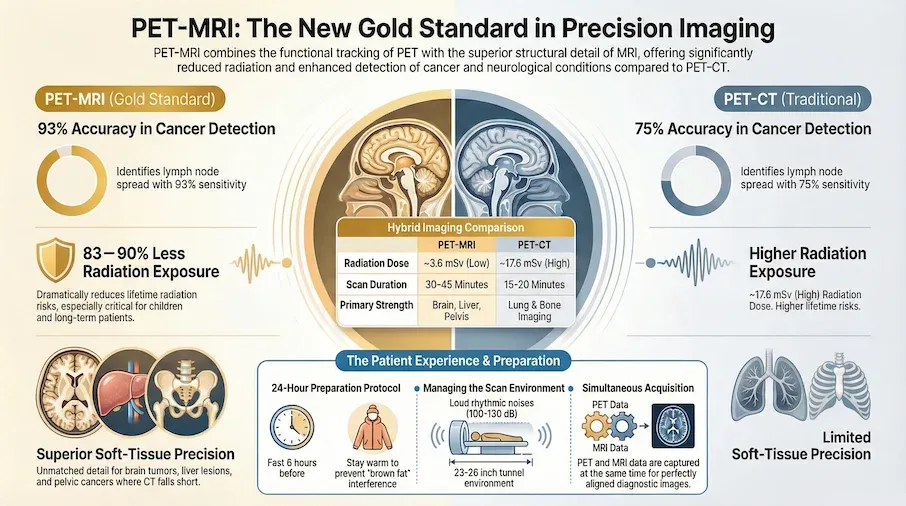
| Radiation Exposure | ~3.6 mSv (PET only; MRI uses no radiation)[Evidence: D][23] | ~17.6 mSv (PET + CT combined) |
| Soft Tissue Detail | Superior for brain, liver, pelvis, bone marrow[Evidence: B][4] | Good overall, superior for lung detail |
| Lymph Node Detection (Colorectal Cancer) | Sensitivity 93%[Evidence: A][3] | Sensitivity 75% |
| Scan Time | 30-45 minutes (longer) | 15-20 minutes (shorter) |
| Availability (US) | ~30 systems (limited) | ~1,600+ systems (widely available) |
| Best Applications | Brain tumors, epilepsy, liver metastases, pediatric cancers, pelvic cancers | Lung cancer, head/neck cancers, lymphoma staging, whole-body surveillance |
| Pediatric Dose Reduction | 83-90% less radiation than PET-CT[Evidence: D][23] | Standard pediatric protocols used |
| Cost | Generally higher (limited availability) | More standardized pricing |
When to Choose PET-MRI
- Pediatric patients (significant radiation dose reduction)
- Patients requiring multiple follow-up scans over time
- Brain tumor evaluation and seizure focus localization
- Liver, pelvic, and soft tissue tumor staging
- Prostate cancer evaluation
- When superior soft tissue contrast is needed
When PET-CT May Be Preferred
- Lung cancer staging (CT provides better lung detail)
- When PET-MRI is not available in your area
- Patients with MRI contraindications (pacemakers, certain implants)
- When faster scan time is clinically necessary
What The Evidence Shows (And Doesn't Show)
What Research Suggests
- Meta-analysis evidence shows PET-MRI detects lymph node spread in colorectal cancer with 93% sensitivity compared to 75% for PET-CT[Evidence: A][3]
- Radiation exposure is reduced by 79.6% compared to PET-CT (3.6 mSv vs 17.6 mSv), with pediatric reductions of 83-90%[Evidence: D][23]
- Integrated approaches combining PSMA PET with MRI improve prostate cancer detection compared to either modality alone[Evidence: B][9]
- Four Level A sources (meta-analyses) and 17 Level B sources (prospective cohorts/RCTs) support clinical utility across multiple cancer types
- Superior soft tissue detail provides incremental diagnostic value for liver, brain, and pelvic tumors compared to PET-CT
What's NOT Yet Proven
- Long-term outcome data comparing PET-MRI vs PET-CT for survival or treatment response is limited. Most studies focus on diagnostic accuracy, not clinical outcomes.
- Optimal protocols for many cancer types are still being established. Different centers may use varying techniques.
- Cost-effectiveness studies comparing PET-MRI to PET-CT are limited, making insurance coverage decisions variable.
- Some newer tracers (TSPO, Fluciclovine, GPC3-targeted) have limited sample sizes (as few as 8 patients) and require larger validation studies.
- SUV quantification differences between PET-MRI and PET-CT (12-42% lower on PET-MRI) mean reference ranges are modality-specific and not interchangeable.
Where Caution Is Needed
- Limited availability (~30 systems in US) means PET-CT may be the practical choice for most patients despite PET-MRI's advantages
- Longer scan times (30-45 min vs 15-20 min) may be challenging for patients with pain, claustrophobia, or difficulty lying still
- PET-CT remains superior for lung imaging due to CT's ability to resolve lung nodules
- Patients with certain metal implants, pacemakers, or severe claustrophobia may not be candidates for PET-MRI
Should YOU Get This Scan?
Best suited for: Patients with brain tumors, epilepsy requiring surgical planning, liver or pelvic cancers, pediatric patients needing serial imaging, prostate cancer evaluation, and any situation where radiation dose minimization is important.
Not recommended for: Patients with non-MRI-compatible pacemakers or implants, severe claustrophobia without sedation option, first trimester pregnancy, or when PET-CT is clinically equivalent and more accessible.
Realistic timeline: Total appointment 2-3 hours. Results typically available within 1-3 business days.
When to consult a professional: Discuss with your ordering physician whether PET-MRI offers advantages over PET-CT for your specific condition. If PET-MRI is recommended, ask for referral to a center with experienced radiologists and simultaneous acquisition technology.
Frequently Asked Questions
I'm on blood thinners. Can I still get a PET-MRI scan?
Yes, blood thinners do not typically prevent you from having a PET-MRI scan. The procedure only requires a standard IV placement, which is safe for patients on anticoagulants. You may have a slightly higher risk of bruising at the injection site. Continue taking your blood thinners as prescribed unless your doctor specifically instructs otherwise. Inform the imaging staff about all medications you take, including blood thinners like warfarin, Eliquis, or Xarelto.
What happens if my MRI shows normal findings but doctors suspect a problem?
Early research suggests TSPO imaging may help detect brain inflammation in epilepsy patients whose standard MRI scans appear normal. The PET component can reveal metabolic abnormalities that MRI alone might miss. Your doctor may recommend additional imaging with different tracers or follow-up scans. The combination of normal anatomical imaging with abnormal metabolic findings provides valuable diagnostic information.
How does PET-MRI help with multiple myeloma staging?
Studies compared three different scan types to find the best way to detect and stage multiple myeloma bone disease. PET-MRI can detect bone marrow involvement and extramedullary disease while providing detailed assessment of soft tissue plasmacytomas. Your oncologist will recommend the most appropriate imaging based on your specific situation and treatment plan.
In men with rising PSA after prostate removal, how does PET-MRI help?
In men with rising PSA levels after prostate removal, this scan helps doctors find where cancer may have returned. PSMA PET combined with MRI provides detailed information about local recurrence and helps guide salvage radiation therapy. Research shows the PRIMARY scoring system helps doctors accurately detect clinically significant prostate cancer using PSMA scans. In men having prostate surgery, PSMA scans matched well with pathology findings.
What does low FDG uptake mean in breast cancer?
In women with estrogen receptor-positive breast cancer, some tumors show lower sugar uptake on FDG scans, which may affect treatment planning. This hypometabolic pattern does not necessarily indicate less aggressive cancer. Your oncologist will interpret your scan results in the context of your tumor biology and recommend appropriate treatment. Additional testing or different imaging tracers may be considered.
Is PET-MRI available for bladder or kidney cancer?
Clinical guidelines discuss the emerging role of this hybrid scan for staging bladder and kidney cancers. While still being integrated into clinical practice, PET-MRI offers advantages for local staging due to superior soft tissue contrast. Clinical guidelines also recommend this scan as one imaging option for evaluating cancers of the mouth and throat. Availability varies by center.
Are there new developments in PET-MRI technology?
Researchers developed a new digital detector insert that allows simultaneous PET and MRI scanning in larger bore systems, tested in animal models. Ongoing research continues to improve image quality, reduce scan times, and expand clinical applications. New radiotracer development expands the conditions PET-MRI can evaluate. Ask your imaging center about their equipment and newest capabilities.
How do blood flow patterns in brain tumors affect PET-MRI results?
In people with brain tumors, blood flow patterns in the tumor can affect how the tracer is taken up, which doctors must consider when interpreting the scan. Specialized radiologists understand these effects and account for them during interpretation. Dynamic scanning protocols that measure changes over time can help distinguish between tumor and treatment effects.
Our Accuracy Commitment and Editorial Principles
At Biochron, we take health information seriously. Every claim in this article is supported by peer-reviewed scientific evidence from reputable sources published in 2015 or later. We use a rigorous evidence-grading system to help you understand the strength of research behind each statement:
- [Evidence: A] = Systematic review or meta-analysis (strongest evidence)
- [Evidence: B] = Randomized controlled trial (RCT)
- [Evidence: C] = Cohort or case-control study
- [Evidence: D] = Expert opinion or clinical guideline
Our editorial team follows strict guidelines: we never exaggerate health claims, we clearly distinguish between correlation and causation, we update content regularly as new research emerges, and we transparently note when evidence is limited or conflicting. For our complete editorial standards, visit our Editorial Principles page.
This article is for informational purposes only and does not constitute medical advice. Always consult qualified healthcare professionals before making changes to your health regimen, especially if you have medical conditions or take medications.
References
- 1 . Comparative efficacy and workflow efficiency of integrated PET/MRI versus sequential PET/CT and MRI in gynecologic cancer staging, Abdominal Radiology (NY), 2025, PubMed [Evidence: B]
- 2 . Head-to-Head Comparison of mpMRI, PSMA, GRPR PET/CT, and PET/CT Plus MRI for Local Staging of Primary Prostate Cancer, Journal of Nuclear Medicine, 2026, PubMed [Evidence: B]
- 3 . Diagnostic Performance of [18F]FDG PET/MRI and [18F]FDG PET/CT in the Detection of Lymph Node Metastases in Colorectal Cancer: A Meta-analysis, World Journal of Nuclear Medicine, 2025, PubMed [Evidence: A]
- 4 . Incremental Value of Digital PET/MRI over PET/CT in the Assessment of Neoplastic Liver Lesions, World Journal of Nuclear Medicine, 2025, PubMed [Evidence: B]
- 5 . Comparison of MRI, [18F]FDG-PET/CT, and [18F]FDG-PET/MRI for Initial Staging of Multiple Myeloma: A Systematic Review and Meta-analysis, Clinical Nuclear Medicine, 2025, PubMed [Evidence: A]
- 6 . Impact of 18F-choline PET-CT or PET-MRI on surgical strategy in patients with primary hyperparathyroidism, BJS Open, 2025, PubMed [Evidence: B]
- 7 . Diagnostic value of 18F-prostate-specific membrane antigen-1007 PET/MRI versus PET/CT for biochemical recurrence of prostate cancer, Nuclear Medicine Communications, 2025, PubMed [Evidence: B]
- 8 . MRI, PET/CT and PET/MRI Fusion in the Assessment of Lymph Node Metastases in Head and Neck Cancer, Diagnostics (Basel), 2026, PubMed [Evidence: B]
- 9 . Combined Prostate-specific Membrane Antigen Positron Emission Tomography and Multiparametric Magnetic Resonance Imaging for the Diagnosis of Clinically Significant Prostate Cancer, European Urology Oncology, 2025, PubMed [Evidence: B]
- 10 . The PRIMARY Scoring System on PSMA PET for Clinically Significant Prostate Cancer Detection: A Systematic Review and Meta-Analysis, Clinical Nuclear Medicine, 2026, PubMed [Evidence: A]
- 11 . Interreader agreement of intraprostatic prostate cancer detection using [18F]PSMA-1007 PET and whole-mount radical prostatectomy specimens, EJNMMI Research, 2026, PubMed [Evidence: B]
- 12 . The proportion, clinical predictors, and prognostic impact of hypometabolic estrogen receptor-positive primary breast cancer on baseline FDG PET, Nuclear Medicine Communications, 2026, PubMed [Evidence: C]
- 13 . Comparing FDG-PET and breast MRI to predict pathological complete response in HER2-positive early breast cancer, ESMO Open, 2025, PubMed [Evidence: B]
- 14 . [18F]FDG PET/MRI in Endometrial Cancer: Prospective Evaluation of Preoperative Staging, Cancers, 2026, PubMed [Evidence: B]
- 15 . Innovative imaging techniques for urothelial carcinoma, Urologie, 2026, PubMed [Evidence: D]
- 16 . Trends in Head and Neck Cancer: Oral Cavity Carcinoma, Radiology: Imaging Cancer, 2025, PubMed [Evidence: D]
- 17 . Glypican-3-Targeted PET Imaging for Precise Diagnosis of Hepatocellular Carcinoma, Clinical Cancer Research, 2026, PubMed [Evidence: C]
- 18 . What is the utility of whole-body PET/MRI in the staging of myxoid liposarcoma?, Skeletal Radiology, 2025, PubMed [Evidence: C]
- 19 . The confounding effects of microvascular physiology on FET-PET accuracy in gliomas, European Journal of Nuclear Medicine and Molecular Imaging, 2026, PubMed [Evidence: B]
- 20 . Differentiating tumor progression from post treatment related change using dynamic 18F-FDG PET-MRI, Zhonghua Yi Xue Za Zhi, 2026, PubMed [Evidence: B]
- 21 . Clinical Utility of [F18]-Fluciclovine PET/MRI for Differentiating True Progression from Treatment-Related Changes in Glioblastoma, AJNR American Journal of Neuroradiology, 2025, PubMed [Evidence: B]
- 22 . Challenges and Innovations in Paediatric Brain Tumour Treatments, Pharmaceutics, 2025, PubMed [Evidence: D]
- 23 . Advances in FDG PET imaging for staging and prognostic assessment in pediatric lymphoma: a systematic review, Pediatric Radiology, 2026, PubMed [Evidence: D]
- 24 . Advanced neuroimaging assessment of neurodegenerative dementia syndromes, NeuroImage Clinical, 2026, PubMed [Evidence: B]
- 25 . Hybrid PET/MRI Imaging of 18F-FDG and TSPO for Presurgical Localization in Refractory Epilepsy, CNS Neuroscience & Therapeutics, 2025, PubMed [Evidence: B]
- 26 . Exploring the Role of TSPO-PET Imaging Among MRI-Negative Patients with Temporal Lobe Epilepsy, Brain Sciences, 2026, PubMed [Evidence: C]
- 27 . Pediatric Huntington Disease Brains Have Distinct Morphologic and Metabolic Traits: the RAREST-JHD Study, Movement Disorders Clinical Practice, 2024, PubMed [Evidence: C]
- 28 . Simultaneous multiple post-labelling delay ASL MRI and [18F]FDG PET in a mixed memory clinic population, European Journal of Nuclear Medicine and Molecular Imaging, 2026, PubMed [Evidence: B]
- 29 . PET-MRI: A New Hybrid Imaging Modality for Dentomaxillofacial Malignancies - A Systematic Review, Diagnostics (Basel), 2025, PubMed [Evidence: D]
- 30 . Initial results of the Hyperion IIDPET insert for simultaneous PET-MRI, Physics in Medicine and Biology, 2025, PubMed [Evidence: C]
Medical Disclaimer
This content is for informational and educational purposes only. It is not intended to provide medical advice or to take the place of such advice or treatment from a personal physician. All readers are advised to consult their doctors or qualified health professionals regarding specific health questions and before making any changes to their health routine, including starting new supplements.
Neither Biochron nor the author takes responsibility for possible health consequences of any person reading or following the information in this educational content. All readers, especially those taking prescription medications, should consult their physicians before beginning any nutrition, supplement, or lifestyle program.
If you have a medical emergency, call your doctor or emergency services immediately.






