Diagnosis and Tests
Breast Ultrasound: Diagnosing Lumps, Cysts vs. Cancer & Dense Tissue

💡 What You Need to Know Right Away
A breast ultrasound is an imaging test that uses sound waves to create detailed pictures of your breast tissue, helping doctors detect lumps, distinguish fluid-filled cysts from solid masses, and guide needle biopsies. The test is safe, painless, and uses no radiation.
Also known as: breast sonography, breast sonogram, breast US, mammary ultrasound, breast echography
- Research shows this test correctly identifies breast cancer in about 8 out of 10 cases when cancer is present[Evidence: A][3]
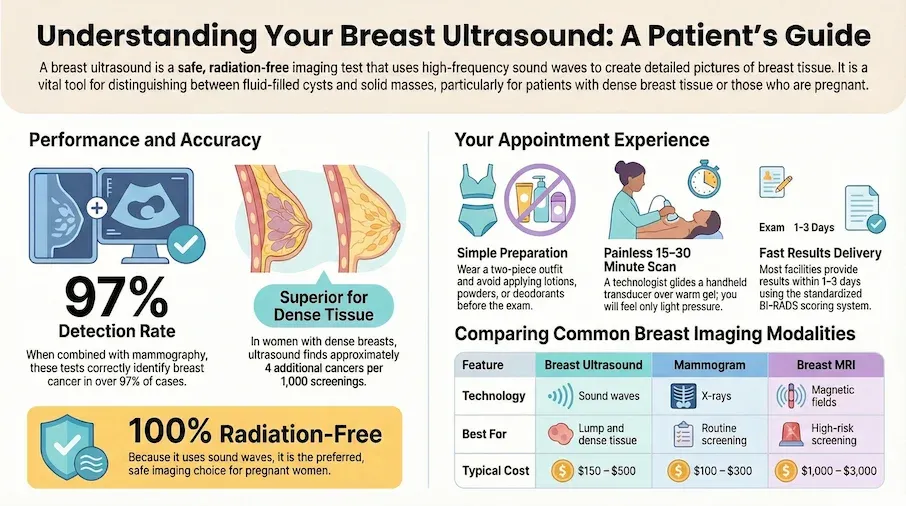
- When combined with mammography, the tests together correctly identify breast cancer in over 97 out of 100 cases[Evidence: B][1]
- In women with dense breasts and negative mammograms, this test finds about 4 additional cancers per 1000 women screened[Evidence: A][4]
- Research shows adding this test to mammography detects 2 additional breast cancers per 1000 women compared to mammography alone[Evidence: A][10]
If your doctor has recommended a breast ultrasound, you may be wondering what to expect and whether you should be concerned. It's normal to feel anxious about any breast imaging test, especially if you've noticed a lump or had an abnormal mammogram.
The good news is that breast ultrasound is one of the safest and most comfortable imaging tests available. Unlike mammograms, there's no breast compression, and unlike X-rays or CT scans, there's no radiation exposure. This makes it particularly valuable for pregnant women, young women under 30, and anyone who needs frequent breast imaging.
In this guide, you'll learn how breast ultrasound works, what it can and cannot detect, how to prepare for your appointment, and how to understand your results. We'll also help you understand when ultrasound is used alongside mammography and when it might be recommended instead.
❓ Quick Answers
What is a breast ultrasound?
A breast ultrasound is a painless imaging test that uses high-frequency sound waves to create pictures of the inside of your breast. The sound waves bounce off breast tissue and are converted into images on a screen. This test helps doctors see the difference between fluid-filled cysts and solid masses, guide needle biopsies, and evaluate lumps found during physical exams or mammograms.
Is breast ultrasound painful?
No, breast ultrasound is not painful. You may feel slight pressure as the technologist moves the transducer (a small handheld device) across your breast, but it should not cause pain. If your breasts are already tender, you may notice mild discomfort, but this is from the underlying tenderness rather than the test itself.
What can a breast ultrasound detect?
Breast ultrasound can detect lumps, cysts, solid masses, and other abnormalities in breast tissue. Research shows this test correctly identifies breast cancer in about 8 out of 10 cases when cancer is present[Evidence: A][3]. It's particularly useful for distinguishing benign fluid-filled cysts from solid masses that may need further evaluation.
Is breast ultrasound safe during pregnancy?
Yes, breast ultrasound is completely safe during pregnancy. It uses sound waves rather than radiation, making it the preferred first-line imaging test for pregnant women with breast concerns. It is also safe during breastfeeding and can be repeated as often as needed without health risks.
How long does a breast ultrasound take?
The ultrasound scan itself typically takes 15 to 30 minutes, depending on the size of your breasts and the areas being examined. Your total appointment time, including check-in, changing into a gown, the scan, and getting dressed, is usually 45 to 60 minutes.
Can breast ultrasound detect cancer?
Yes, breast ultrasound can detect many breast cancers. When combined with mammography, the tests together correctly identify breast cancer in over 97 out of 100 cases[Evidence: B][1]. However, ultrasound is typically used alongside mammography rather than as a replacement, especially for routine breast cancer screening.
Breast Ultrasound
A non-invasive diagnostic tool using high-frequency sound waves to visualize the internal structure of breast tissue. Essential for targeted screening and diagnostic clarity.
🔬 How Does Breast Ultrasound Work?
Breast ultrasound works by sending high-frequency sound waves into your breast tissue using a small handheld device called a transducer. Think of it like sonar on a submarine: the sound waves travel through your breast, bounce off different structures, and return to the transducer. A computer then translates these echoes into real-time images on a screen.
Different types of breast tissue create different echoes. Fluid-filled structures like cysts appear dark (called "anechoic" in medical terms) because sound waves pass right through liquid. Solid tissues like tumors or normal glandular tissue appear lighter because they reflect more sound waves back. Imagine dropping a pebble into a pond versus a bucket of sand: the water barely disrupts the ripple, while the sand creates a strong echo. This is how ultrasound distinguishes between harmless cysts and solid masses that may need further testing.
Research confirms that breast ultrasound is effective at early detection. In women with dense breasts, adding ultrasound to mammography helps detect additional breast cancers and reduces the number of cancers that appear between screenings[Evidence: B][2]. Studies indicate that supplementary ultrasound imaging leads to about 5 additional breast cancers per 1000 women being diagnosed when added to digital mammography[Evidence: A][11].
The test also provides real-time imaging, which makes it invaluable for guiding needle biopsies. Doctors can watch the needle on the screen as they position it precisely into a suspicious area, improving accuracy and safety.
In people whose breast cancer was found by this test, 98 out of 100 were cancer-free after 5 years[Evidence: B][1][Evidence: C][6]. This favorable outcome reflects that ultrasound-detected cancers are often found at earlier, more treatable stages.
Breast ultrasound has also proven effective in resource-limited settings, where it serves as an accessible and affordable early detection method[Evidence: C][7].
🧪 What to Expect: The Real User Experience
During the Procedure
You'll lie on your back on an exam table, with your arm raised above your head on the side being examined. This position may feel awkward if held for 15 or more minutes and can cause shoulder tiredness. The room is typically dimmed so the technologist can see the screen clearly, but it's not dark. Unlike an MRI, there's no enclosed space, so claustrophobia is not a concern.
The technologist applies a clear, water-based gel to your breast. If not warmed, the gel can feel noticeably cool when first applied, causing some patients to flinch. Many facilities now use gel warmers, which makes the gel feel like warm lotion. The gel has a slippery consistency similar to hand sanitizer but thicker.
The transducer, about the size of a computer mouse with a smooth surface, is then moved across your breast. You'll feel light to moderate pressure as it glides over your skin. The pressure may be firmer when examining specific areas of concern. If your breasts are tender (such as during your premenstrual week or if you have fibrocystic breasts), you may notice more discomfort, but sharp pain is not normal.
What You'll Feel After
There are no physical aftereffects. You won't experience bruising, soreness, swelling, or fatigue. You may notice slight stickiness if the gel wasn't fully wiped off. This washes off easily with soap and water. You can immediately return to driving, work, and exercise with no recovery period needed.
Many people feel relieved that the procedure is over, while others feel anxious waiting for results. Results are typically available same day or within 1-3 days.
How to Make It Easier
- For tender breasts: Schedule your appointment during days 7-14 of your menstrual cycle if possible, when breasts are typically less tender
- If gel feels cold: Ask the technologist if they have a gel warmer
- For shoulder discomfort: Let the technologist know if the arm-above-head position becomes uncomfortable; they can briefly reposition
- To stay calm: Focus on breathing or ask questions to distract yourself ("What are you seeing on the screen?")
- Important to know: Many technologists cannot discuss findings during the exam because a radiologist reviews the images later. Silence does not mean bad news
📊 How to Prepare for Your Breast Ultrasound
Breast ultrasound requires minimal preparation, but a few simple steps can make your appointment smoother and more comfortable.
| Preparation Step | Why It Matters | Timing |
|---|---|---|
| Wear a two-piece outfit (separate top and bottom) | You'll only need to remove your top; easier than changing entirely | Day of appointment |
| Skip lotion, powder, and deodorant on your breasts and underarms | These products can interfere with ultrasound imaging quality | Morning of appointment |
| Remove jewelry (necklaces, body piercings) | Metal can create image artifacts | Before entering exam room |
| Bring insurance card and ID | Required for check-in and billing | Day of appointment |
| Bring prior imaging results if from a different facility | Allows radiologist to compare with previous images | Confirm with facility beforehand |
| Note any breast concerns to mention (lumps, pain, changes) | Helps technologist focus on areas of concern | Before appointment |
What You Can Do Normally
- Eating and drinking: No fasting required. Eat and drink normally before your appointment.
- Medications: Continue taking all medications as prescribed.
- Activities: No restrictions before or after the test.
Procedure Timeline
Check-in and paperwork: 5-10 minutes → Change into gown: 2-3 minutes → Gel application and scan: 15-30 minutes → Gel removal and dressing: 5 minutes → Total visit time: 45-60 minutes
⚠️ Safety, Limitations, and What to Know
Breast ultrasound is one of the safest medical imaging tests available. The test uses sound waves, not radiation, so there are no known health risks from diagnostic ultrasound. It's safe during pregnancy, while breastfeeding, and can be repeated as often as needed.
What Ultrasound Does Well
- Distinguishes fluid-filled cysts from solid masses
- Evaluates lumps found during physical exam or mammography
- Guides needle biopsies with real-time imaging
- Screens women with dense breast tissue alongside mammography
- Provides imaging without radiation for pregnant or young women
Limitations to Understand
While ultrasound is highly valuable, it has important limitations. Clinical guidelines from the US Preventive Services Task Force state that current evidence is insufficient to determine whether the benefits of supplemental screening with ultrasound outweigh the potential harms[Evidence: D][8].
Research shows that adding ultrasound to mammography results in more false alarms, with about 37 more women per 1000 called back unnecessarily compared to mammography alone[Evidence: A][10]. Research also shows that handheld ultrasound had the highest rate of callbacks and false alarms when used as supplemental screening[Evidence: A][11].
Ultrasound cannot detect all breast cancers, particularly small calcifications that mammography can identify. It is not recommended as a standalone replacement for screening mammography in most women.
When to Contact Your Doctor
- You notice a new breast lump or changes in breast shape
- You have nipple discharge (especially bloody)
- Your ultrasound results show something suspicious (BI-RADS 4 or 5)
- You have ongoing breast pain that doesn't improve
- You have a strong family history of breast cancer and want to discuss screening options
🥗 Practical Tips for Your Breast Ultrasound
Before Your Appointment
- Choose the right timing: If your breasts are typically tender before your period, schedule during days 7-14 of your cycle when possible
- Dress strategically: A button-front shirt or loose top makes changing easier and faster
- Bring a companion: If you're feeling anxious, having someone in the waiting room can provide support
- Write down your questions: Prepare questions for your doctor about results and next steps
During Your Appointment
- Communicate openly: Tell the technologist if pressure is uncomfortable or if you have specific areas of concern
- Stay still during scanning: Movement can blur images; take slow, steady breaths
- Ask about gel temperature: Request warmed gel if the cold gel is uncomfortable
After Your Appointment
- Ask about timeline: Find out when to expect results and how you'll receive them (phone call, patient portal, follow-up visit)
- Keep copies: Request a copy of your ultrasound images if you see multiple doctors or may change providers
- Schedule follow-ups: If recommended, schedule your next imaging appointment before leaving
Understanding Your Results
Breast ultrasound results are reported using the BI-RADS (Breast Imaging Reporting and Data System) categories:
- BI-RADS 1: Negative (no abnormalities)
- BI-RADS 2: Benign (definitely not cancer, such as simple cysts)
- BI-RADS 3: Probably benign (short-term follow-up recommended)
- BI-RADS 4: Suspicious (biopsy recommended)
- BI-RADS 5: Highly suspicious for malignancy (biopsy strongly recommended)
- BI-RADS 6: Known cancer (biopsy already confirmed)
What to Look for When Choosing a Breast Ultrasound Provider
The quality of your ultrasound results depends on the imaging facility and the professionals performing and interpreting the test. Here's what to consider:
Facility Quality Markers
- ACR accreditation: American College of Radiology (ACR) accreditation indicates quality standards are met Why it matters: ACR-accredited facilities undergo rigorous evaluation of equipment, personnel, and procedures
- Board-certified radiologists: Verify radiologists are certified by the American Board of Radiology Why it matters: Board certification confirms specialized training in breast imaging
- Dedicated breast imaging center: Facilities specializing in breast imaging often have more experienced staff Why it matters: Higher procedure volume typically correlates with more accurate readings
- Modern equipment: Ask if the facility uses current-generation ultrasound equipment Why it matters: Newer equipment provides better image resolution
Questions to Ask Your Provider
- Is your facility ACR-accredited for breast ultrasound?
- Who will interpret my ultrasound images?
- When will I receive my results, and how?
- Do you have my prior mammogram or ultrasound images for comparison?
- What is the cost if my insurance doesn't fully cover it?
- Do you offer same-day biopsy if needed?
Red Flags
- No ACR accreditation: Non-accredited facilities may lack quality oversight
- Results delayed more than 1 week: Most facilities provide results within 1-3 days
- No radiologist interpretation: Images should be read by a board-certified radiologist, not just the technologist
- Unable to provide cost estimate: Reputable facilities can provide pricing information upfront
How Breast Ultrasound Compares to Mammogram and MRI: What to Know
Breast ultrasound, mammography, and MRI are complementary tools, each with unique strengths. Understanding the differences helps you and your doctor choose the right test for your situation.
| Feature | Breast Ultrasound | Mammogram | Breast MRI |
|---|---|---|---|
| How It Works | Sound waves create images | Low-dose X-rays compress breast tissue | Magnetic fields and radio waves create detailed images |
| Radiation Exposure | None | Low dose | None |
| Best For | Evaluating lumps, dense breasts, guiding biopsies, pregnancy | Routine screening, detecting calcifications | High-risk screening, pre-surgery planning |
| Sensitivity (Standalone) | About 80%[Evidence: A][3] | Varies by breast density | Highest sensitivity |
| Additional Cancers Detected | 4.2-4.3 per 1000 (when added to mammogram)[Evidence: A][4] | Primary screening method | 17.4 per 1000 (interim data)[Evidence: B][5] |
| Comfort Level | No compression; most comfortable | Breast compression can be uncomfortable | Requires lying still in enclosed tunnel |
| Duration | 15-30 minutes | 10-20 minutes | 30-60 minutes |
| Typical Cost (Without Insurance) | $150-$500 | $100-$300 | $1,000-$3,000 |
| Limitations | Cannot detect calcifications; operator-dependent | Less effective in dense breasts | Expensive; more false positives; contrast required |
Automated Breast Ultrasound (ABUS) vs Handheld
A newer technology called Automated Breast Ultrasound System (ABUS) uses a machine to scan the entire breast, reducing operator variability. Studies suggest that automated 3D breast ultrasound correctly identifies breast cancer in about 92 out of 100 cases, compared to 83 out of 100 for handheld ultrasound[Evidence: C][9].
In women aged 50-70 with dense breasts and negative mammograms, automated breast ultrasound detected about 4 additional cancers per 1000 women[Evidence: B][5]. The recall rate (being called back for additional testing) was about 5 out of 100 women[Evidence: C][9].
Which Test Is Right for You?
- Routine screening (average risk, age 40+): Mammogram is the standard first-line screening test
- Dense breasts with negative mammogram: Ultrasound may be recommended as supplemental screening
- Evaluating a specific lump or concern: Ultrasound is often the first additional test
- High risk (BRCA mutation, strong family history): MRI often recommended alongside mammography
- Pregnant or under age 30: Ultrasound is typically preferred due to no radiation
What The Evidence Shows (And Doesn't Show)
What Research Suggests
- When combined with mammography, breast ultrasound helps identify breast cancer in over 97 out of 100 cases[Evidence: B][1]
- In women with dense breasts, adding ultrasound to mammography detects about 4 additional cancers per 1000 women screened[Evidence: A][4]
- Research from a Cochrane systematic review shows combined screening detects 2 additional breast cancers per 1000 women (5.0 vs 3.2 per 1000 with mammography alone)[Evidence: A][10]
- In women with dense breasts, about 3 additional cancers per 1000 are detected with combined screening[Evidence: A][10]
- In people whose breast cancer was found by ultrasound, 98 out of 100 were cancer-free after 5 years[Evidence: B][1][Evidence: C][6]
What's NOT Yet Proven
- Whether supplemental ultrasound screening reduces breast cancer mortality (long-term survival data from screening trials is limited)
- Optimal screening intervals for supplemental ultrasound (annual vs. other frequencies not definitively established)
- Whether the benefits of supplemental screening outweigh the harms, including unnecessary biopsies from false positives
- The value of ultrasound screening in populations other than those with dense breasts and negative mammograms
Where Caution Is Needed
- Adding ultrasound to mammography increases false positives: about 37 more women per 1000 are called back unnecessarily[Evidence: A][10]
- Handheld ultrasound has the highest recall and false positive rates among supplemental imaging methods[Evidence: A][11]
- The USPSTF concludes evidence is insufficient to determine the balance of benefits and harms of supplemental screening[Evidence: D][8]
- Ultrasound results are operator-dependent; quality can vary between facilities and technologists
Should YOU Get a Breast Ultrasound?
Best suited for: Women with dense breast tissue, those evaluating a palpable lump or mammogram abnormality, pregnant women needing breast imaging, women under 30 with breast symptoms, and those guiding needle biopsy procedures
Not recommended for: Primary breast cancer screening as a standalone test in average-risk women (mammography is preferred)
Realistic expectations: Ultrasound is excellent for distinguishing cysts from solid masses and finding additional cancers in dense breasts, but it cannot replace mammography for routine screening
When to consult a professional: Before deciding on supplemental screening, if you're unsure whether you have dense breasts, if you have a breast lump or symptom, or if you're at high risk due to family history or genetic factors
Frequently Asked Questions
Do I need to undress for a breast ultrasound?
You will need to remove your top and bra for the examination. You'll be given a gown that opens in the front. Only the breast being examined will be exposed at any time, and the technologist will drape you to maintain your privacy. Wearing a two-piece outfit (separate top and bottom) means you won't need to remove your pants or skirt.
How much does a breast ultrasound cost?
Without insurance, a breast ultrasound typically costs $150-$500 depending on your location and the facility. With insurance, you may pay a copay ($10-$50) or coinsurance (10%-50% of the allowed amount). If your ultrasound is ordered to evaluate a symptom (like a lump), it's considered diagnostic and insurance typically covers it. Some states mandate coverage for supplemental breast imaging in women with dense breasts. Contact your insurance company before your appointment to understand your coverage.
Can I eat before a breast ultrasound?
Yes, you can eat and drink normally before a breast ultrasound. No fasting is required. This test only images your breast tissue and is not affected by what's in your stomach. Continue taking all medications as prescribed unless your doctor specifically instructs otherwise.
What should I wear to a breast ultrasound?
Wear a two-piece outfit with an easy-to-remove top. A button-front shirt is ideal. Avoid one-piece dresses or rompers. Skip jewelry around your neck or chest area. Don't apply lotion, powder, or deodorant to your breasts or underarms on the day of your appointment, as these products can interfere with the ultrasound images.
What does an abnormal breast ultrasound mean?
An 'abnormal' ultrasound result doesn't automatically mean cancer. It means the radiologist found something that needs further evaluation. This could be a benign cyst, a fibroadenoma (benign solid mass), or an area that needs additional imaging or biopsy. The BI-RADS category in your report indicates the level of concern: BI-RADS 3 means probably benign with short-term follow-up recommended, while BI-RADS 4 or 5 indicates a biopsy is recommended to determine if the finding is cancerous.
Can breast ultrasound miss cancer?
Yes, breast ultrasound can miss some cancers. Research shows this test correctly identifies cancer in about 8 out of 10 cases when cancer is present. Ultrasound is less effective at detecting tiny calcifications, which can be an early sign of certain cancers. This is why ultrasound is typically used alongside mammography rather than as a replacement. If you have a concerning lump that ultrasound shows as 'normal,' discuss additional testing with your doctor.
Does insurance cover breast ultrasound?
Most insurance plans cover breast ultrasound when it's medically necessary, such as evaluating a lump or following up on an abnormal mammogram. Coverage for supplemental screening ultrasound (when you have no symptoms but have dense breasts) varies by state and insurance plan. Some states mandate coverage for supplemental imaging in women with dense breasts. Medicare covers diagnostic breast ultrasound when ordered by a doctor to investigate a symptom or finding. Contact your insurance company before your appointment to verify coverage.
Is breast ultrasound safe for breastfeeding?
Yes, breast ultrasound is completely safe during breastfeeding. The test uses sound waves, not radiation, and does not affect breast milk production or quality. You do not need to pump and dump after an ultrasound. If you notice a breast lump while breastfeeding, ultrasound is often the first imaging test recommended because it can distinguish between milk-filled ducts, cysts, and other findings common during lactation.
How accurate is breast ultrasound?
Research shows breast ultrasound has pooled sensitivity of about 80% (correctly identifies cancer when present) and specificity of about 88% (correctly rules out cancer when absent). When combined with mammography, sensitivity increases to over 97%. Accuracy can vary based on operator experience, equipment quality, and breast density. Automated breast ultrasound (ABUS) may have higher sensitivity than handheld ultrasound.
Can breast ultrasound replace mammogram?
For most women, breast ultrasound cannot replace mammogram as a primary screening tool. Mammography remains the standard for routine breast cancer screening because it can detect calcifications and early-stage cancers that ultrasound may miss. However, ultrasound plays important complementary roles: screening women with dense breasts, evaluating lumps, and imaging pregnant or very young women where avoiding radiation is preferred. Your doctor can help determine the best imaging strategy for your individual situation.
Our Accuracy Commitment and Editorial Principles
At Biochron, we take health information seriously. Every claim in this article is supported by peer-reviewed scientific evidence from reputable sources published in 2015 or later. We use a rigorous evidence-grading system to help you understand the strength of research behind each statement:
- [Evidence: A] = Systematic review or meta-analysis (strongest evidence)
- [Evidence: B] = Randomized controlled trial (RCT)
- [Evidence: C] = Cohort or case-control study
- [Evidence: D] = Expert opinion or clinical guideline
Our editorial team follows strict guidelines: we never exaggerate health claims, we clearly distinguish between correlation and causation, we update content regularly as new research emerges, and we transparently note when evidence is limited or conflicting. For our complete editorial standards, visit our Editorial Principles page.
This article is for informational purposes only and does not constitute medical advice. Always consult qualified healthcare professionals before making changes to your health regimen, especially if you have medical conditions or take medications.
References
- 1 . Ultrasound as the Primary Screening Test for Breast Cancer: Analysis From ACRIN 6666, Journal of the National Cancer Institute, 2015, PubMed [Evidence: B]
- 2 . Sensitivity and specificity of mammography and adjunctive ultrasonography to screen for breast cancer in the Japan Strategic Anti-cancer Randomized Trial (J-START), Lancet, 2016, PubMed [Evidence: B]
- 3 . Ultrasound for Breast Cancer Detection Globally: A Systematic Review and Meta-Analysis, Journal of Global Oncology, 2019, PubMed [Evidence: A]
- 4 . Supplemental Breast Cancer Screening in Women with Dense Breasts and Negative Mammography: A Systematic Review and Meta-Analysis, Radiology, 2023, PubMed [Evidence: A]
- 5 . Comparison of supplemental breast cancer imaging techniques-interim results from the BRAID randomised controlled trial, Lancet, 2025, PubMed [Evidence: B]
- 6 . Breast Cancer Detected at Screening US: Survival Rates and Clinical-Pathologic and Imaging Factors Associated with Recurrence, Radiology, 2017, PubMed [Evidence: C]
- 7 . Evaluating the Role of Breast Ultrasound in Early Detection of Breast Cancer in Low- and Middle-Income Countries: A Comprehensive Narrative Review, Bioengineering, 2024, PubMed [Evidence: C]
- 8 . Screening for Breast Cancer: US Preventive Services Task Force Recommendation Statement, JAMA, 2024, PubMed [Evidence: D]
- 9 . Diagnostic performance of 3D automated breast ultrasound (3D-ABUS) in a clinical screening setting-a retrospective study, European Radiology, 2024, PubMed [Evidence: C]
- 10 . Mammography in combination with breast ultrasonography versus mammography alone in women at elevated risk of breast cancer, Cochrane Database of Systematic Reviews, 2023, PubMed [Evidence: A]
- 11 . Examining the effectiveness of supplementary imaging modalities for breast cancer screening in women with dense breasts: A systematic review and meta-analysis, European Journal of Radiology, 2022, PubMed [Evidence: A]
Medical Disclaimer
This content is for informational and educational purposes only. It is not intended to provide medical advice or to take the place of such advice or treatment from a personal physician. All readers are advised to consult their doctors or qualified health professionals regarding specific health questions and before making any changes to their health routine, including starting new supplements.
Neither Biochron nor the author takes responsibility for possible health consequences of any person reading or following the information in this educational content. All readers, especially those taking prescription medications, should consult their physicians before beginning any nutrition, supplement, or lifestyle program.
If you have a medical emergency, call your doctor or emergency services immediately.






